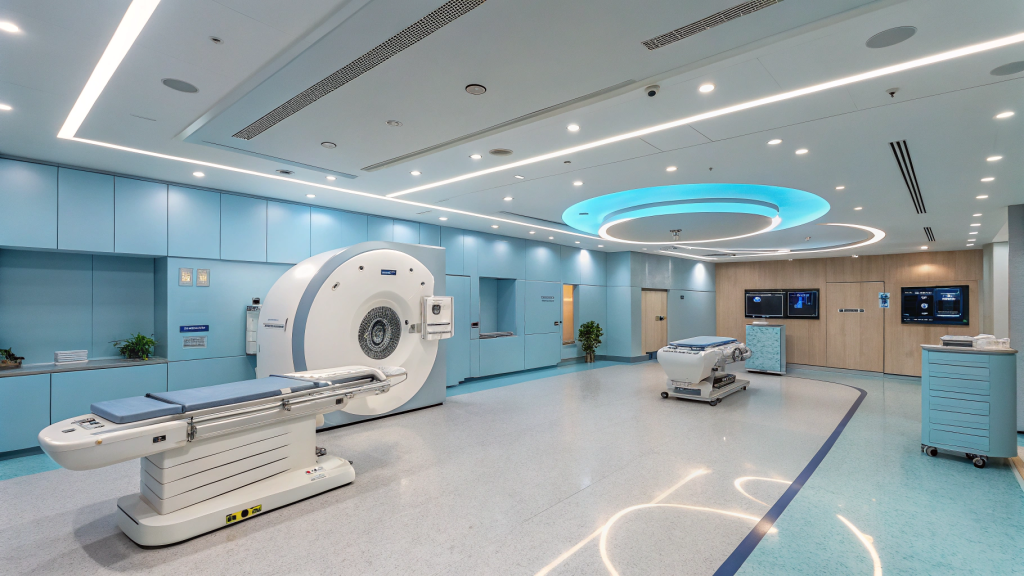
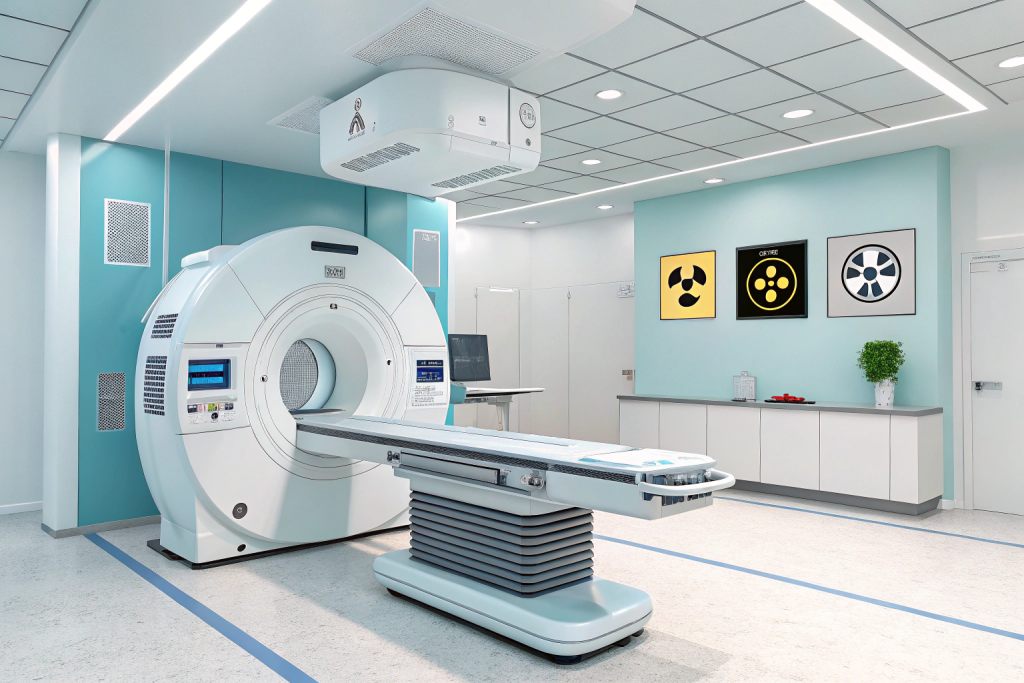
Positron Emission Tomography combined with Computed Tomography, known as PET/CT, is a powerful imaging tool used widely in the diagnosis, staging, and treatment monitoring of various medical conditions—especially cancer. Despite its increasing usage, many patients and even some caregivers still harbor misconceptions about this highly effective diagnostic technology.
In this blog post, we will debunk the most common myths associated with PET/CT scans and offer expert explanations that clarify how the technology really works. Understanding the truth behind these misunderstandings is essential not only for peace of mind but also for ensuring better cooperation with your healthcare providers during the diagnostic journey.
Misconception 1: PET/CT Scans Are Only for Cancer Diagnosis
One of the most widespread beliefs is that PET/CT scans are used exclusively to detect cancer. While this assumption is understandable—given the scan’s popularity in oncology—it is not entirely accurate.
Expert Clarification:
PET/CT is indeed a key tool in cancer detection and management. However, it is also used in cardiology, neurology, and even infectious disease diagnosis. For example, it can help evaluate brain disorders such as Alzheimer’s disease, identify areas of inflammation or infection, and assess heart muscle viability after a heart attack.
Therefore, saying that PET/CT is only for cancer limits the broader understanding of its diagnostic capabilities.
Misconception 2: The Radiation Exposure Is Extremely Dangerous
Another major concern among patients is that PET/CT exposes them to harmful levels of radiation. This fear often leads to reluctance in undergoing the scan, even when it is medically necessary.
Expert Clarification:
While it’s true that PET/CT involves exposure to ionizing radiation, the amount is generally low and well within international safety guidelines. The benefits of accurate diagnosis, staging, and treatment planning far outweigh the minimal risks associated with this temporary radiation.
In fact, many experts emphasize that avoiding medically indicated scans due to radiation fear can lead to missed or delayed diagnoses, which are far more dangerous.
Consequently, patients are advised to follow their doctor’s recommendations rather than avoiding the scan out of fear.
Misconception 3: PET and CT Are the Same Thing
Patients often confuse PET and CT scans, assuming they are interchangeable or that they serve the same purpose.
Expert Clarification:
Although both are imaging technologies, PET and CT perform different functions. CT (Computed Tomography) provides detailed anatomical images, showing the structure of organs and tissues. PET (Positron Emission Tomography), on the other hand, captures metabolic and functional information, highlighting how tissues and organs are functioning.
When combined, PET/CT scans offer both anatomical and metabolic information in a single image, allowing for more precise diagnosis. This integration, therefore, makes the scan more effective than using either modality alone.
Misconception 4: PET/CT Scans Are Painful or Invasive
Many patients worry that the PET/CT procedure will be painful, uncomfortable, or even invasive.
Expert Clarification:
A PET/CT scan is non-invasive and painless. The most discomfort a patient might feel is a small needle prick when a radioactive tracer is injected intravenously. After the injection, patients typically rest for 30–60 minutes while the tracer circulates in the body. Then, the scan itself takes around 20–30 minutes, during which the patient lies still on a table.
Thus, while the procedure may require some patience, it does not involve pain or surgical intervention.
Misconception 5: All Tracers Are Radioactive and Harmful
The idea of injecting a radioactive substance can understandably cause alarm. Many believe that all tracers are dangerous and could potentially harm the body.
Expert Clarification:
PET/CT uses radioactive tracers in extremely small amounts, typically less than what one is exposed to during a long-haul flight. The most commonly used tracer is FDG (fluorodeoxyglucose), which mimics glucose and accumulates in active tissues—especially cancer cells.
These tracers are quickly eliminated from the body through urine and pose minimal to no long-term health risks. As a result, they are considered safe for the vast majority of patients.
Misconception 6: Diabetic Patients Cannot Have PET/CT Scans
Some people believe that diabetic patients are not eligible for PET/CT scans due to glucose-related tracers.
Expert Clarification:
Diabetes can affect how FDG is absorbed, but it does not exclude patients from undergoing PET/CT. Physicians usually adjust preparation protocols—such as fasting hours or insulin schedules—to ensure accurate results.
Therefore, rather than avoiding the scan, diabetic patients should simply inform their care team so that appropriate measures can be taken.
Misconception 7: The Scan Results Are Always 100% Accurate
Many individuals place complete trust in the scan’s results, believing that PET/CT provides infallible answers.
Expert Clarification:
Although PET/CT is among the most advanced imaging technologies available, no diagnostic tool is 100% accurate. False positives and negatives can occur due to a variety of factors, including inflammation, infections, or technical limitations.
That being said, PET/CT scans are highly sensitive and specific when interpreted by experienced radiologists. They should always be considered alongside clinical history, lab tests, and other imaging results for a comprehensive diagnosis.
Misconception 8: You Can Eat Normally Before a PET/CT Scan
Another widespread myth is that there are no dietary restrictions before the scan.
Expert Clarification:
In most cases, patients are required to fast for at least 4–6 hours before the scan, especially when FDG is used. Eating before the scan can alter glucose metabolism, which may affect the tracer’s distribution and skew the results.
Because of this, it is critical to follow your healthcare provider’s preparation instructions carefully.
Final Thoughts: Trust the Science, Not the Myths
In summary, while PET/CT technology continues to evolve and benefit countless patients around the world, misconceptions can still create unnecessary fear and confusion. These myths—ranging from radiation concerns to inaccurate assumptions about scan eligibility—can lead patients to delay or even reject important diagnostic evaluations.
Therefore, being well-informed and seeking clarification from medical professionals is essential. Expert radiologists, nuclear medicine physicians, and oncology teams are trained to guide you through the process safely and transparently.
Ultimately, trust in science, clear communication, and collaboration with your care team will ensure that you get the most accurate, timely, and effective diagnostic support possible.